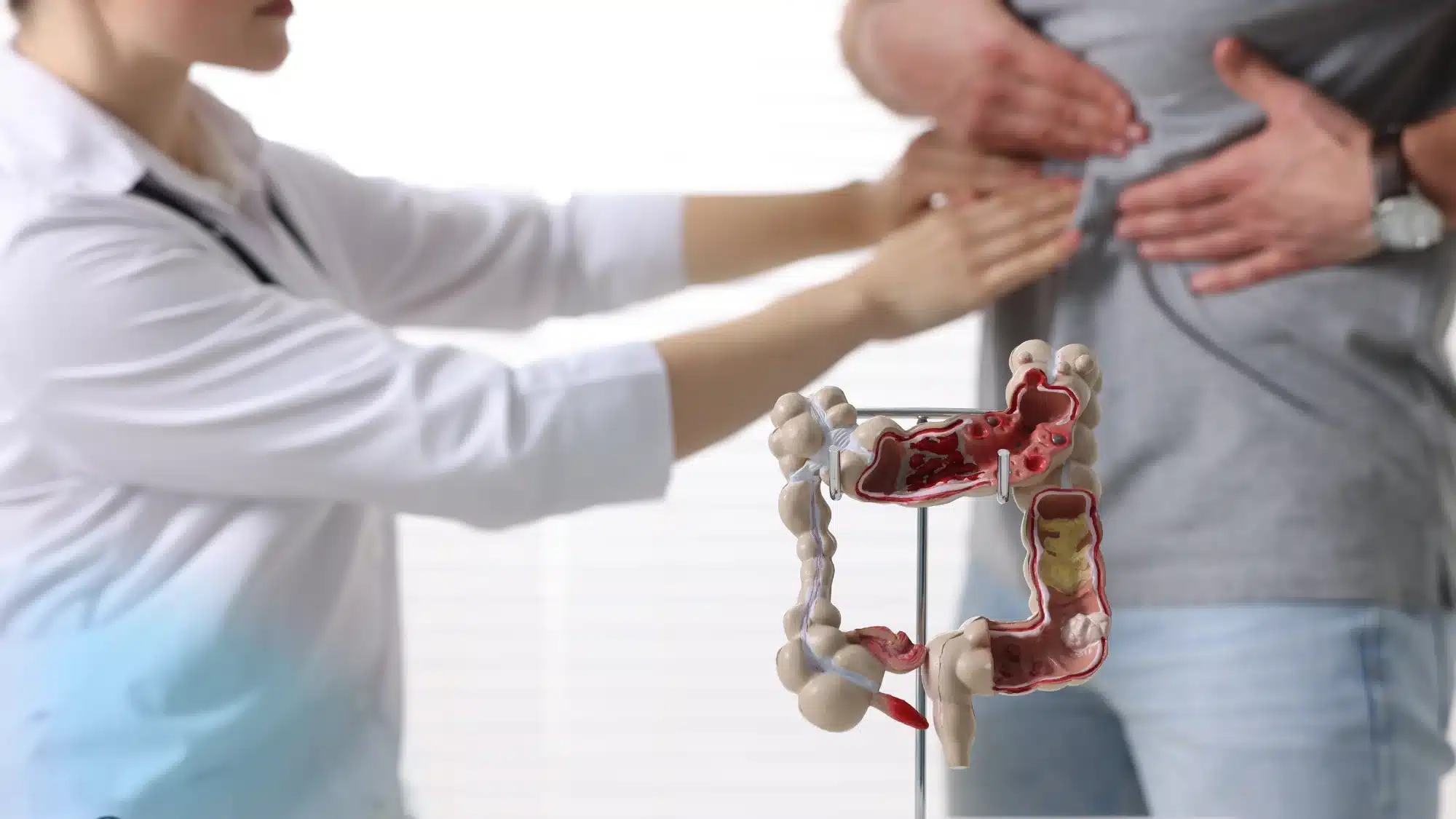
If you’re trying to search for a “gastroenterologist near me,” you’ll want to know how your insurance coverage affects visits to a GI practice. Insurance plans vary widely, but understanding common patterns can help you plan and avoid unexpected costs. This guide outlines how coverage typically works for gastroenterology office visits and related procedures.
Understanding Your Plan’s basics
- In-network vs out-of-network: Most plans offer better coverage when you see an in-network gastroenterologist near me. Out-of-network care can result in higher deductibles, coinsurance, or even balance bills in some situations.
- Copays, deductibles, and coinsurance: An office visit often has a copay or coinsurance, and you may also have a deductible that must be met before your plan pays a larger share. Some plans apply costs differently for specialists, depending on whether the visit is considered preventive or diagnostic.
- Primary care referral requirements: Some insurance plans require a referral from your primary care physician to see a gastroenterologist near me, while others allow direct access to specialists. Check your plan documents or contact your insurer to confirm requirements.
Office Visits versus Procedures
- Office visit billing: A gastroenterology office visit is typically billed under an evaluation and management (E/M) code. Your payment responsibility at the time of service could be a copay or coinsurance, depending on your plan.
- Procedures and tests: Many GI visits lead to tests or procedures (e.g., endoscopy, colonoscopy, biopsies, or imaging) that have separate charges. These may be billed by the physician and by the facility where the procedure occurs, and coverage can differ for the office visit versus the procedure itself.
- Pathology and sedation: If tissue samples are taken (biopsies) or if sedation is used during a procedure, pathology fees and anesthesia-related costs may apply in addition to the physician’s charge.
Preventive vs Diagnostic Colonoscopy
- Preventive (screening) colonoscopy: Many plans cover screening colonoscopy with no out-of-pocket cost if you meet age criteria and there are no symptoms or indications requiring diagnostic testing.
- Diagnostic colonoscopy: If you have symptoms (e.g., bleeding, abdominal pain) or a known GI issue, the colonoscopy is generally considered diagnostic. In many cases, deductible, coinsurance, and sometimes a separate facility fee apply.
- If polyps are found and removed: The procedure may involve additional charges for biopsy, pathology, or polypectomy, and the coverage may differ from a simple screening exam.
No Surprises Act: Protections under the No Surprises Act help limit surprise balance billing for certain out-of-network services, but coverage details depend on plan type and service location. Not all scenarios are guaranteed to be fully covered without cost-sharing.
Practical Steps to Verify Coverage
- Review plan documents and the Summary of Benefits to understand in-network vs out-of-network coverage, deductibles, co-pays, and coinsurance.
- Contact the insurer to verify benefits for a gastroenterology office visit, colonoscopy, or related tests with the intended provider.
- Ask for a benefits verification or an estimated cost sheet that separates the office visit, procedure, anesthesia, and any pathology or facility fees.
- Confirm any pre-authorization requirements for procedures and whether the clinic or facility can assist with cost estimates.
- Bring your current insurance card to every appointment and keep receipts and explanations of benefits for your records.
Tips for a smoother experience
- If you’re searching for a “gastroenterologist near me,” consider asking whether the practice can help with upfront cost estimates and benefit checks.
- If you’re approaching a visit with possible procedures, plan around your deductible and out-of-pocket maximum so you aren’t surprised by larger charges later in the year.
- Discuss payment plans or financing options if you anticipate higher costs due to necessary testing or procedures.
Understanding how insurance coverage typically applies to gastroenterology office visits can help you navigate costs more confidently when you search “gastroenterologist near me”. For patients of Merus Gastroenterology & Gut Health LLC, if you have questions about your benefits, contact your insurer for a benefits verification and speak with our administrative team to simplify estimates and scheduling. By staying informed and planning ahead, you can focus on your gut health with greater peace of mind. If you’re ready to take the next step, schedule a visit with a gastroenterologist near you and discuss coverage options openly with the care team.